Flashes & Floaters
Sydney Eye Surgeons ophthalmologists have extensive training and expertise in the diagnosis and management of posterior vitreous detachments.
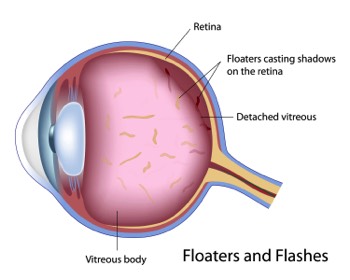
The back of the eye is full of a gel known as vitreous. With time this gel breaks down and becomes liquefied. This is a normal process and can occur at anytime. As the vitreous liquefies it breaks away from the retina. This is known as a Posterior Vitreous Detachment (PVD).
How are PVDs treated?
Patients usually present with a sudden onset of floaters in front of their vision. A floater moves with the patient and occasionally disappears from view. A PVD is a normal event that occurs with age and does not need to be treated.
Patients become accustomed to the floater and often the brain ‘adapts’ so it is rarely seen. Rarely a floater can become very bothersome.
What are the complications of a PVD?
In a small percentage of patients with PVDs as the vitreous pulls away from the retina a small tear is formed. If a retinal tear occurs patients will usually notice and increase in floaters, flashing lights to the side or a curtain over their visual field.
A small retinal tear is treated with laser in the rooms to seal the break. Topical anaesthetic is instilled into the eye and a contact lens inserted to visualise the break. Laser is then applied. Patients tolerate this very well. Follow up is required to check the tear is sealed.
Occasionally a retinal tear results in a retinal detachment if fluid tracks beneath the retina at the point of the break. This is more common in myopic or short sighted people. This requires surgery to repair. This has a very high success rate with modern techniques.
If you would like an assessment regarding retinal vein occlusion, please call our rooms or make an online enquiry.
BONDI JUNCTION
Park Place
Suite 601, Level 6
3 Waverley Street
Bondi Junction NSW 2022
02 9387 4427
Fax: 02 9388 0139
Directions and parking
HURSTVILLE
Suite 12, Level 2
33 MacMahon Street
Hurstville NSW 2220
02 9579 4004
Fax: 02 9570 1377
Directions and parking
HOURS
Monday to Friday
8:30am until 5:00pm
FOR PATIENTS
FOR REFERRERS
© 2017- SYDNEY EYE SURGEONS














