Diagnostic Tests
These are some of the diagnostic tests that may be performed depending on your ophthalmologist's assessment.
Digital Photography
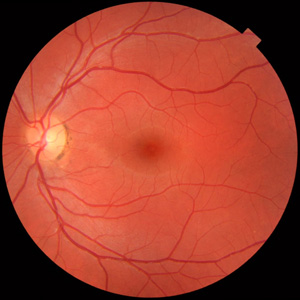
A specialised digital camera is used to photograph the back of the eye(fundus). Your doctor may then explain your eye condition better by showing you pictures of your eye on the computer screen. Fundus photography is used to assess diabetes, glaucoma, blocked arteries or veins and many other retinal conditions. They also provide a snapshot of what your fundus looks like at a particular point in time, allowing comparison with subsequent visits.
Photos can also be taken of the front part of the eye to record corneal, conjunctival and iris lesions for example.
FFA (Fluorescein Angiography)
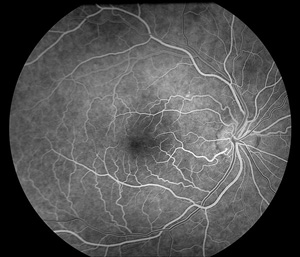
Fluorescein dye injected into a vein in your hand travels to the eye through its blood vessels. Photographs are taken in rapid succession to record its passage through the eye's circulation. Abnormal blood vessels and blood flow, as well as conditions affecting the retina such as diabetic eye disease and choroidal neovascularization in macular degeneration can be diagnosed and better treated.
OCT (Optical Coherence Tomography)
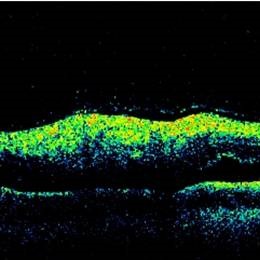
OCT or optical coherence tomography images the architecture of the back of the eye with reflected light. A high resolution cross-sectional view of the retina is provided, along with accurate measurement of the optic nerve fibre layer in glaucoma. OCT allows your doctor to accurately assess whether further treatment is required for your macular condition or glaucoma, as comparisons over time can be made.
Visual Field Analysis
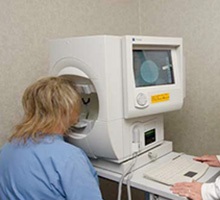
Visual field analysis checks your side vision which can be affected by glaucoma. It is also useful to diagnose many other eye disorders, especially those affecting the visual pathway. It involves pressing a button when flashes of light are seen and requires good concentration. For glaucoma patients it is usually performed every 6 months, or 12 months if the glaucoma is well controlled.
A-Scan and Keratometry

These are measurements and calculations to work out what power intraocular lense implant is required if you are having cataract surgery. The tests are customized for your eye and visual requirements. Keratometry measures the curvature of the front of your eye, and whether there is any astigmatism. If there is significant astigmatism, this can be corrected with a special intraocular lense implant, a Toric implant.
The A-scan measures the length of the eye as well, it provides other measurements of the distance between structures withing the eye. A computer programme is used to calculate the power of the intraocular lens with these two measurements, taking into consideration the type of implant required.
Biopsy
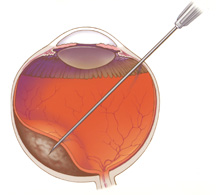
This is performed to determine the diagnosis of a conjunctiva or eyelid lesion. Local anaesthesia is used to numb the area involved and a small sample of tissue is excised and sent to the pathology lab for examination. This is often done in the day procedure room in our surgery. Results may take a couple of weeks to return or longer if special stains are required. An accurate diagnosis would help determine the best management for the eye condition involved.
Gonioscopy
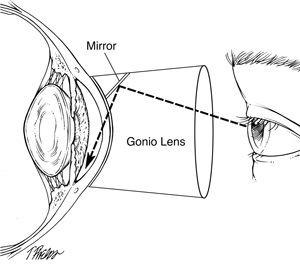
Gonioscopy is often done as part of the examination for glaucoma screening. A handheld contact lens is used to view the area between the iris and cornea. Topical anaesthesia is instilled in the the eye and the gel applied to the lens surface before placing it gently on the eye. If glaucoma is present, viewing the angle will help determine whether it is primary open angle glaucoma or angle closure glaucoma.
BONDI JUNCTION
Park Place
Suite 601, Level 6
3 Waverley Street
Bondi Junction NSW 2022
02 9387 4427
Fax: 02 9388 0139
Directions and parking
HURSTVILLE
Suite 12, Level 2
33 MacMahon Street
Hurstville NSW 2220
02 9579 4004
Fax: 02 9570 1377
Directions and parking
HOURS
Monday to Friday
8:30am until 5:00pm
FOR PATIENTS
FOR REFERRERS
© 2017- SYDNEY EYE SURGEONS














